Intro: Understanding our body’s immunological response to coronavirus infection in the mouth and nose may hold the key to an effective vaccine
New Delhi, Have you ever wondered what is it that keeps several people healthy and asymptomatic even after they have caught the scary novel coronavirus? Well, the answer might lie in our mucosal immune system, according to scientists at University at Buffalo.

In a new paper published in the Frontiers in Immunology argue that unravelling
how immunity emerges to SARS-CoV-2 (the virus that causes COVID disease) in the mucous membranes of the nose and mouth may lead to the development of a more effective and easy-to-administer vaccine.
“Given that many infected people remain asymptomatic, and that a large number of those who develop symptoms suffer only mild to moderate disease, this suggests that something, somewhere, does a fairly good job of controlling the virus,” said Michael W. Russell, emeritus professor, Department of Microbiology and Immunology at UB, and senior author on the paper.
“Could it be that this is due to early mucosal immune responses that succeed in containing and eliminating the infection before it becomes serious?” he asked. “We will not know unless these questions are addressed.”
Russell noted that naturally, the initial focus of research on the disease was on cases of severe disease when the virus descends into the lower respiratory tract, especially the lungs, where the cellular immune responses exacerbate the inflammation rather than fight the infection.
But since the upper respiratory tract, including the nose, tonsils and adenoids are the initial point of infection for the SARS-CoV-2 virus, the immune responses that are triggered there are of special interest.
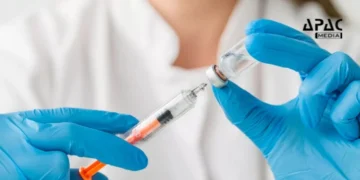
Major pharma companies the world over are working on COVID vaccines. Most vaccines use a protein component of the virus. The non-protein vaccines use the nucleic acid of the virus and require cold storage.
Moderna and Pfizer-BioNTech vaccines are nucleic acid based vaccines. But Pfizer vaccine requires a storage temperature of minus 70 degrees, which is impractical in countries like India.
The Serum Institute of India is collaborating with the Oxford-AstraZeneca vaccine, which uses spike protein.
The UB scientists argue that a focus on mucosal immunity might also make it possible to develop a type of vaccine, such as a nasal vaccine, that could be easier to store, transport and administer.
Russell added that these vaccines might not have special temperature requirements and might be more palatable for large swaths of the population, especially children, because they would not require an injection.















































Discussion about this post